Women, kids as prone to hernia as men
A hernia occurs when an organ pushes through an opening in the muscle or tissue that holds it in place. For example, the intestines may break through a weakened area in the abdominal wall. Though it is usually believed that hernias mostly occur in men, women and children are also, if not equally, at risk. Hernias are most common in the abdomen, but they can also appear in the upper thigh, belly button, and groin areas. An untreated hernia will not go away on its own, hence it is important to recognize the early signs of a hernia. With lifestyle changes and early medical care, one can minimize the effects of hernia and avoid life-threatening complications like strangulation.
Types
Inguinal hernia
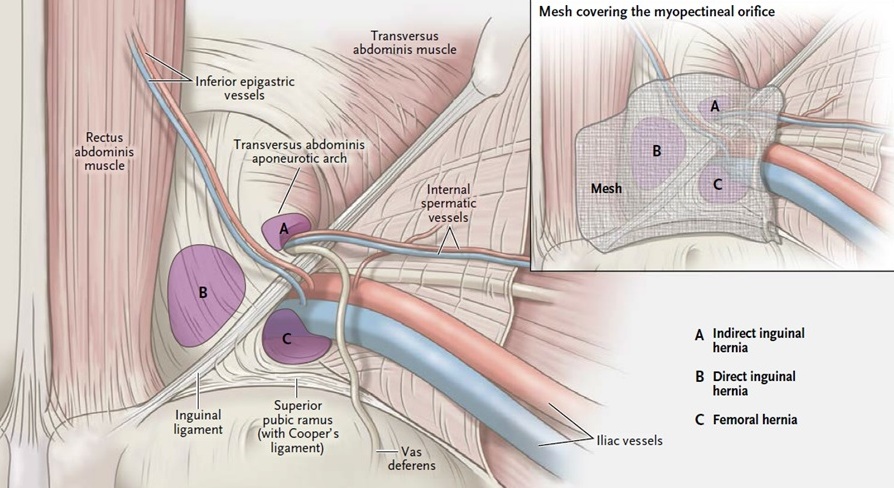
Inguinal hernias are the most common type of hernia. Indirect inguinal hernias develop due to the natural weakness in the internal inguinal ring. These hernias occur when the intestines push through a weak spot or tear in the lower abdominal wall, often in the inguinal canal. The inguinal canal is found in the groin. In men, it is the area where the spermatic cord passes from the abdomen to the scrotum. This cord holds up the testicles. In women, the inguinal canal contains a ligament that helps hold the uterus in place. This type of hernia is more common in men than in women. This is because a man’s testicles descend through the inguinal canal shortly after birth, and the canal is supposed to close almost completely behind them. Sometimes, the canal does not close properly and leaves a weakened area prone to hernias.
Hiatal hernia
A hiatal hernia occurs when part of the stomach protrudes up through the diaphragm into the chest. The diaphragm is a sheet of muscle that helps one breathe by contracting and drawing air into the lungs. It separates the organs in the abdomen from those in the chest. This type of hernia is most common in patients over 50 years of age. If a child has the condition, it’s typically caused by a congenital (birth) defect. Hiatal hernias almost always cause gastroesophageal reflux, which is when the stomach contents leak backward into the esophagus, causing a burning sensation.
Umbilical hernia
Umbilical hernias occur near the bellybutton or navel, which has a natural weakness from the blood vessels of the umbilical cord. These hernias may occur in infants at or just after birth, and may resolve at three or four years of age. However, the area of weakness can persist throughout life and can occur in women, men, and children at any time. In adults, umbilical hernias will not resolve and may progressively worsen over time. They are sometimes caused by abdominal pressure due to being overweight, excessive coughing, or pregnancy.
Incisional hernia
Ventral hernias are also called incisional hernias. These hernias can appear at the site of a previous surgery weeks, months, or even years later and can vary in size from small to very large and complex. If ventral hernias are left untreated, they may widen and become extremely difficult to repair.
Femoral hernias
Femoral hernias are rare but occur almost exclusively in women. These hernias appear just below the groin crease and are usually the result of pregnancy and childbirth. A weakness in the lower groin allows an intestinal sac to drop into the femoral canal, a space near the femoral vein that carries blood from the leg. These hernias are more prone to develop incarceration or strangulation as an early complication than are inguinal hernias. Therefore, once these hernias are diagnosed, early repair is very strongly advised before such complications occur.
Causes
Hernias are caused by a combination of muscle weakness and strain. Depending on its cause, a hernia can develop quickly or over a long period of time. Common causes of muscle weakness include: failure of the abdominal wall to close properly in the womb, which is a congenital defect, age, chronic coughing or damage from injury or surgery. Factors that strain the body and may cause a hernia, especially if the muscles are weak, include: being pregnant, which puts pressure on the abdomen; being constipated, which causes one to strain when having a bowel movement, lifting heavy weight, fluid in the abdomen, suddenly gaining weight and persistent coughing or sneezing.
Who is at Risk?
The factors that increase the risk of developing a hernia include: Personal or family history of hernias, being overweight or obese, a chronic cough, chronic constipation, smoking, which can trigger a chronic cough. Conditions such as cystic fibrosis can also indirectly increase the risk of developing a hernia. Cystic fibrosis impairs the function of the lungs, causing a chronic cough.
Symptoms
The most common symptom of a hernia is a bulge or lump in the affected area. In the case of an inguinal hernia, you may notice a lump on either side of the pubic bone where the groin and thigh meet. You’re more likely to feel the hernia through touch when you’re standing up. If the baby has a hernia, you may only be able to feel the bulge when he or she is crying. A bulge is typically the only symptom of an umbilical hernia. Other common symptoms of an inguinal hernia include: Pain or discomfort in the affected area (usually the lower abdomen), especially when bending over, coughing, or lifting, weakness, pressure, or a feeling of heaviness in the abdomen, a burning, gurgling, or aching sensation at the site of the bulge, acid reflux, which is when stomach acid moves backward into the esophagus causing a burning sensation, chest pain, difficulty swallowing. In some cases, hernias have no symptoms. You may not know you have a hernia unless it shows up during a routine physical or a medical exam for an unrelated problem.
Diagnosis
Inguinal or incisional hernias are usually diagnosed through a physical examination. The doctor may feel for a bulge in the abdomen or groin that gets larger when you stand, cough, or strain. If you have a hiatal hernia, the doctor may diagnose it with a barium X-ray or endoscopy. These tests allow the doctor to see the internal location of the stomach. If the child has an umbilical hernia, the doctor may perform an ultrasound.
Treatment
Whether or not you need treatment depends on the size of the hernia and the severity of the symptoms. The doctor may simply monitor the hernia for possible complications. Treatment options for a hernia include lifestyle changes, medication or, if the hernia is growing larger or causing pain, the doctor may decide that it’s best to operate.
Complications
If left untreated, the hernia may grow and become more painful. A portion of the intestine could become trapped in the abdominal wall. This can obstruct the bowel, causing severe pain, nausea, and constipation. An untreated hernia can also put too much pressure on nearby tissues, which can cause swelling and pain in the surrounding area. If the trapped section of the intestines doesn’t get enough blood flow, strangulation occurs. This can cause the intestinal tissue to become infected or die. A strangulated hernia is life-threatening and requires immediate medical care.
Prevention
You can’t always prevent the muscle weakness that allows a hernia to occur. However, you can reduce the amount of strain you place on the body. This may help you avoid a hernia or keep an existing hernia from getting worse. Prevention tips include: Not smoking, seeing the doctor when you’re sick to avoid developing a persistent cough, maintaining a healthy body weight, avoiding straining during bowel movements or urination, lifting objects with the knees and not the back, avoiding lifting weights that are too heavy for you.
May 2017
Understanding ulcers of the stomach
Stomach ulcers are painful sores that can be found in the stomach lining or small intestine. Stomach ulcers are the most visible sign of peptic ulcer disease. They occur when the thick layer of mucus that protects your stomach from digestive juices is reduced, thus enabling the digestive acids to eat away at the lining tissues of the stomach. Their symptoms are not only painful, but can also lead to complications, such as infections, changes in appetite and ongoing nausea/vomiting.
Causes
For many years, doctors thought that high amounts of stress alone could cause a stomach ulcer to form by increasing production of stomach acid, but then research emerged in the 1980s showing that frequent use of anti-inflammatory drugs (NSAIDs like aspirin), a poor lifestyle and a type of bacterial infection caused by the strain Helicobacter pylori (H. pylori) were more likely to be the real culprits of ulcers. Genetic hyperacidity and Zollinger-Ellison syndrome, a rare disease that makes the body produce excess stomach acid, may also cause ulcers. Certain factors and behaviours that can put you at higher risk for developing stomach ulcers include: Smoking; frequent use of steroids (such as those for treating asthma); hypercalcemia (overproduction of calcium); family history of stomach ulcers; being over 50 years old; excessive consumption of alcohol. Stomach ulcers are easily cured, but they can become severe without proper treatment.
Complications
Seek treatment as soon as you believe that you might have a stomach ulcer. The longer an ulcer remains untreated, the more likely you are to develop complications. You should seek medical treatment if you experience any of the following symptoms: sudden, sharp pain that doesn’t stop; black or bloody stools; bloody vomitus or vomit that looks like coffee grounds. These could be signs that the ulcer has eroded through the stomach, or broken a blood vessel. Scar tissue development is another possible complication. The tissue can prevent food from moving from the stomach into the small intestine. All of these scenarios require intensive therapy, usually in a hospital setting.
Symptoms
The most common stomach ulcer symptoms include: abdominal pains and burning sensations (especially after eating and between the belly and breastbone); bleeding when vomiting or going to the bathroom; nausea and vomiting; darker stools; loss of appetite and changes in body weight; trouble sleeping due to pain; other digestive complaints like heartburn, acid reflux, feeling gassy; the risk for perforation of the organ lining (a life-threatening condition requiring emergency surgery to repair small openings in the lining of the GI tract); dehydration, weakness and fatigue.
How ulcers work
When someone has an ulcer, hydrochloric acid and pepsin (a type of digestive enzyme that digests proteins) build up and destroy parts of the lining of the gastrointestinal tract. The stomach usually manages acid/pepsin by creating a thick mucus coating that is supposed to act as a buffer between the stomach lining and the acids inside the stomach. The mucus coating itself usually produces certain chemicals that help repair the stomach lining, keep blood circulating and carry out cellular renewal processes. But some part of this process can become disturbed, and the lining of the GI tract can become exposed, forming small sores (ulcers). When you eat a meal, food washes the acid in your stomach away temporarily as it’s used to break down the nutrients in the recently consumed food. But then once your food is digested, the acid once again accumulates in the stomach and can wash against the “raw base” of the ulcer, exposing and opening it up. This causes a burning, painful sensation, sometimes one that’s very strong.
Preventions
1. Limit Use of NSAID Pain Relievers: People of any age who take NSAIDs every day or multiple times per week are more likely to develop stomach ulcers and heartburn compared to people who don’t take them very often. NSAIDs (like aspirin) are prescribed very often to treat all sorts of conditions that cause a fever, pain and swelling — and some people rely on taking them practically every day to help control their chronic or reoccurring pain (such as headaches, arthritis/joint pain, PMS cramps, muscle tears, infections, colds and so on). NSAIDs affect the gastrointestinal system by altering how digestive enzymes and stomach acids are produced. There are two enzymes that produce chemicals in your body that promote pain, inflammation and fever. NSAIDs not only decrease these enzymes, but at the same time lower production of another chemical that protects the stomach lining from stomach acid.​ If you can, stop taking the NSAIDs or at least greatly reduce how much of them you take regularly. Taking antacids for a stomach ulcer might help ease pain temporarily, but it will keep coming back if the underlying issue causing the ulcer isn’t resolved.
2. Manage Stress: Although the theory that stress alone causes stomach ulcers is no longer fully supported, stress still plays a part in the development of ulcers, and the condition is still considered somewhat “psychosomatic.” When someone experiences chronic stress, the risk for a stomach ulcer goes up, since there’s a strong “gut-brain connection” involved in normal digestive processes. The body easily picks up on perceived threats and changes how digestion is carried out, which is why a very high percentage of people with anxiety/depression experience some sort of digestive illness or complaints. People with anxiety and high amounts of stress have been observed to have higher than normal rates of ulcers and more frequent infections. Stress weakens the immune system and worsens digestion, making it more likely you become sick from various bacteria or microbes you come into contact with.
3. Boost Immunity and Control Inflammation: A highly inflammatory lifestyle weakens the immune system and makes the digestive system more susceptible to an infection caused by H. pylori bacterium. H. pylori itself can then cause even more inflammation within the stomach and small intestine, creating a vicious cycle that’s hard to break. H. pylori contributes to ulcers by damaging the mucous coating that protects the lining of the stomach and duodenum from acids. Once damaged, stomach acid is able to get through to the sensitive lining, causing burning and irritation. H. pylori can be spread through unclean water, food or utensils, plus through bodily fluids (like saliva) — but it’s only likely to cause an ulcer when someone’s immunity is low for other reasons.
4. Improve Lifestyle: Boost protection against infections by dropping poor lifestyle habits like smoking, drinking high amounts of alcohol, eating a poor diet high in processed foods, toxin exposure and a sedentary lifestyle — which favour inflammation, lower immunity and contribute to ulcer formation. Some of these can also make treatment of ulcers more difficult. For example, research shows that smoking cigarettes makes ulcers harder to heal and possibly more painful.
5. Eat Low-Processed, Nutrient-Dense Diet: An improper diet that includes lots of packaged, processed foods and few fresh foods (like vegetables and fruit) raises the risk for ulcers by promoting inflammation and hindering immune functions. Skipping regular meals and eating only one to two times per day but a large amount of food at once can also make ulcer symptoms worse. So maybe skipping breakfast isn’t the best idea. Some people also find that eating spicy foods makes their symptoms worse (although this depends on the person and doesn’t affect everyone).Foods most frequently associated with gastric discomfort include: black pepper; black salt; red or hot pepper and chilli powder; caffeine; regular and decaffeinated coffee or tea; alcohol; cocoa, chocolate and cola beverages; citrus fruits and juices; fatty and fried foods; tomato products and peppermint.
If your ulcer causes nausea and vomiting, it’s important to prevent dehydration, electrolyte imbalances and nutrient deficiencies. Some people with painful ulcers wind up eating less overall in order to avoid pain/burning and therefore risk not consuming enough calories and nutrients. The likelihood for inflammation and deficiencies is even higher if the food being consumed is low in vitamins, minerals and antioxidants to begin with.
Other tips related to your diet to help control ulcers include: maintaining a healthy weight and avoiding obesity; avoiding common stomach irritants and allergies to test your reactions (such as gluten and dairy products).
Diagnosis
To rule out H. pylori infection, a blood, stool, or breath test may be ordered. In a breath test, you’ll be instructed to drink a clear liquid and breathe into a bag, which is then sealed. If H. pylori is present, the breath sample will contain higher-than-normal levels of carbon dioxide. Other tests and procedures used to diagnose stomach ulcers include: Barium enema: a thick white liquid (barium) that you drink helps the stomach and small intestine show up on X-rays; Endoscopy: a thin, lighted tube is inserted through the mouth and into the stomach to look for the presence of an ulcer. Endoscopic biopsy: a piece of stomach tissue is removed so it can be analyzed.
Treatment
Most ulcers can be treated with a prescription from your doctor, but in rare cases, surgery may be required.
March-April 2017
High temperatures cause stomach upsets & nausea
The weather has changed very abruptly and the cases of upset stomach and nausea are pouring in. In March, very high temperatures usually witnessed during peak summer months are creating a great deal of discomfiture for people. Dehydration may be a common effect but the worst hit is the stomach. Many people are witnessing discomfort in the stomach, which is usually accompanied by the urge to vomit. The causes could be food poisoning or poor digestion. During hot days of the year, the risks of stomach pain dramatically increase, since we are more exposed to heat stress and micro-organisms that thrive during warm days in undercooked foods. Too much pain causes nausea and vomiting. Suppose there is undigested food lying in your stomach and rotting, you will experience pain and the body’s natural mechanism will be to flush it out in the form of vomit. However, too much vomiting causes dehydration and loss of vital salts that need to be replenished.
Most common causes
Large and improper meals (too fatty and spicy foods, eating late in evenings), inadequate amounts of water intake, sun exposure and staying at high temperatures or travelling too much can cause upset stomach and nausea. Food poisoning, infections of the stomach and intestines are thus common during the summer season and cause nausea and stomach aches. However, it should be borne in mind that persistent nausea for no apparent reason may be a warning signs of serious health problems, such as appendicitis and obstruction (blockage) of intestines, changes in the mucosa of the stomach or intestines (ulcers, various types of cancer).
Why is nausea frequent during summer
The answer to this question is very simple - nausea occurs due to inadequate nutrition. If you are a fan of fatty meat, salty and spicy food, and late meals, there is a good chance that you will have more stomach problems than people who opt for smaller meals consisting of raw fruits and vegetables, soups, well cooked meals. The reason is that the temperature stress is pushing our bodies to the limit of endurance. If you add the effort that your stomach is investing to digest heavy meals - it is clear that there will be difficulties with digestion, and that the sickness after eating is inevitable. These problems are further intensified if you have gone through hard physical labour. Nausea accompanied by heartburn, vomiting, bloating, and gas is the consequence of poor summer menu.
In summers, food poisoning is common
Due to the high temperature at day and night, summer is ideal for the growth of microorganisms. If the food is kept in inadequate and unhygienic way it may become contaminated. The causes of food poisoning usually belong to one of three groups of bacteria:
•Salmonella: The most common causes of infection are contaminated meat and eggs. Symptoms of poisoning (nausea, fever, abdominal pain, vomiting and diarrhoea) begin 12 to 24 hours after taking the contaminated food. Most often the disease lasts a few days and with proper diet passes. Sometimes vomiting and diarrhoea lead to dehydration of the body.
•Staphylococci: The food, mostly ice cream and mayonnaise, are contaminated with these bacteria and symptoms are caused by toxins - by-products of the work of these bacteria. The first symptoms appear after three to six hours, in the form of abdominal pain, severe nausea, vomiting and diarrhoea. Body temperature may be slightly increased, but the disease after 12 to 24 hours withdraws without any complications.
•Clostridia: Spores of Clostridium botulinum secrete toxins that cause a potentially fatal condition. It can be found in canned food, and poisoning symptoms (headache, nausea and malaise are followed by vomiting and diarrhoea, blurred vision or double images, muscle weakness and sometimes paralysis) occurs 12 to 36 hours after consuming contaminated food.
Prevention is reflected in good hygiene in the kitchen when preparing food and storing food, washing hands and avoiding high-risk foods. In case of poisoning, it is necessary to introduce appropriate dietary regime, drinking plenty of water and seek a physician to assess the situation and determine further treatment.
Sunstroke & heat stroke
Long exposure of head to sun launches a defence mechanism of our body that aims to cool the brain. The body sends more blood in the overheated brain, causing a dilation of blood vessels that causes severe headaches, increase in body temperature, nausea and stomach malaise, a feeling of confusion, ringing in the ears, visual disturbances, dizziness. Heat stroke may not necessarily be the result of exposure to the sun, but can occur due to high temperature in the car or near some machines. In such circumstances, the symptoms are similar to sunstroke, except that the body temperature rises to 40 degrees, leading to disturbances in the central nervous system. These are potentially very serious conditions, but during the hottest part of the day you should remain in the shade, avoid heavy manual labour and take plenty of water.
Motion sickness
Even though we call it ‘motion sickness’, symptoms that are manifested by nausea, dizziness and vomiting, and often are accompanied by the drop in blood pressure and exhaustion, may occur in the movement of every vehicle. Travel sickness is also called the syndrome of bad adaptation to movement or motion sickness, and its main cause is quite natural inability of the brain to process the large amount of information, causing a gap between stimuli that receive and hear the reaction of the body. This causes an imbalance - dizziness, nausea and even vomiting. For example, on the winding road the brain processes the information that eye sends and tries to align it with movements in order to react against the force which is exposed to the body. This instinctive "resisting" to inertia results in disturbances in the stomach.
Nausea is not dangerous, but vomiting is
Summer sickness by itself is not dangerous and its treatment actually represents the elimination of the causes. If problems occur due to poisoning, when the number of microorganisms in the body decreases, their impact on the digestive system will decrease, so the nausea will alleviate, if they are incurred as a result of sickness, everything will go back to normal soon after the cessation of movement. Sunstroke and heatstroke are acute conditions that last for several days, and are treated by cooling the body and drinking a lot of water, in order to restore normal body thermoregulation.
However, because the nausea is usually preceded by vomiting, this condition should not be ignored. Frequent vomiting, especially during the hottest days, can cause dehydration and shock, which is potentially a very dangerous situation. It is therefore necessary for the correct hydration of the organism (the consumption of sufficient amounts of water, or use infusion solutions).
Feb 2017
Colour of your urine is important health indicator
People experience many physiological changes during the times of the year when one season merges into another or, simply put, winters give way to summers and vice versa. In fact, you may experience one or more of over 40 different symptoms associated with weather changes. In other words, a changing weather can stress out your immune system, making you more vulnerable to infections and viruses.
Common health problems that occur due to weather changes include fatigue, stress, skin irritation or rashes, loss of appetite and cough. So, how can you prevent weather-related illnesses? It is important that you boost your immune system. A healthy and well-balanced person is seldom sensitive to a sudden weather change. If you are a healthy and strong person, you can actually endure the stress caused by weather changes and not show any signs of discomfort or sickness. Try to keep your house clean and free from dust as much as possible to remove the allergens. Avoid cigarette smoking as well as eating strong spicy food.
Then, Vitamin C is definitely an immune system booster. It is also effective in the prevention of colds and flu, or to quickly recover from an illness. Because vitamin C is water soluble, it enters the bloodstream directly and your kidneys can excrete the excess vitamin when needed. Vitamin C and other water-soluble vitamins are not stored in the body so you need to replenish it continuously.
Like it is important to partake nutritional food, it is equally or even more important to flush out the waste from our bodies. This waste is excreted through urine and stools. Kidneys filter out the waste products from the blood into the urine that is formed in the kidneys. The useful or essential nutrients are retained in the blood. This process is called reabsorption. This process is very important for a healthy body. However, when certain useful products such as protein or red blood cells start to get excreted through urine, it is not a normal condition. Thus, we can say that the colour of the urine is an important health indicator. It is an indicator of kidney diseases or other conditions prevailing in the body. Thus the colour, smell and consistency of urine can tell a lot about the condition of our body. If we have an idea, we can get a signal about the changing health status of our body. For example, a straw yellow colour is the colour of healthy urine. However, often urine colour change can be attributed to how much or how little water we have been drinking. The other factors that can affect the colour of the urine are food and some medications. But the colour of urine should return to its normal once the medication is stopped.
Here are the different shades of urine and what they indicate:
Transparent: Clear urine is usually a sign of being well-hydrated. However, in some cases it can signal that you might be drinking too much and are risking water intoxication. Over-hydration means that you are drinking more than you need and you might be harming your body by overly diluting the salts. This doesn't usually cause any serious health issues, but just don't force yourself to drink beyond what you need.
No Colour At All: Having a more transparent urine colour can be an indictor of diabetes. If your urine has no colour at all, this can also be a sign of diabetes. The other symptoms include constant thirst and frequent urination. If you feel you need to drink all the time, you must take a diabetes test. No colour of your urine is also an important health indicator.
Pale Straw to Amber or Honey: A straw yellow colour is the colour of healthy urine. As the colour becomes darker, this can be an indicator that you are becoming dehydrated and need to drink liquids. When your urine gets more concentrated, this is usually accompanied by a stronger odour. Some foods can also make your urine dark yellow. For example beet roots can make your urine darker.
Syrup or Brown: Brown coloured urine can be a symptom of an underlying condition. People with liver disease can have brown urine. If your liver is not working properly, the bile salts that should be eliminated with faeces might be excreted through urine as their concentration in blood is high. Hepatitis, an inflammation of the liver, is an example of a liver condition that colours pee dark. It can also be a sign of dehydration so you might need to get it checked by a doctor.
Pink to Reddish: Red colour can come from blood in the urine, a condition known as hematuria. Red is usually the most alarming colour. Red urine causes are many such as urinary tract infections, stones in the kidneys and bladder or some cancers of the kidney, prostate or bladder can all cause bleeding and colour your urine red. Urination can be accompanied by pain in these cases and it might be difficult to urinate. Red or pink urine colour can also come from certain foods and substances you ingested, so you need to rule this out first. Foods that give urine a red shade include beets, blackberries and rhubarb. If colour change is not due to any food and it happens more than once, this can also signal that there is a serious health problem.
Blue Colour: There is also a rare condition known as porphyria. This is an inherited enzyme condition that can make the person's urine blue or purple. However, urine can have a bluish tinge to it. This is most commonly caused by certain foods and medications that contain dyes. The medications which cause your urine to become blue are triamterene (a mild diuretic) or Viagra use.
Green: If there is some pus in the urine, this can make it green-looking. Urinary tract infections are the most common cause of that. This can also be caused by food such as asparagus is the main culprit. You will also notice a distinct smell after you've eaten it. It can also be due to eating black licorice or any food that contains strong colourings which don't get absorbed in your intestines. Medications can also make your urine greenish such as some antibiotics.
Foamy Urine: It may be caused by the presence of proteins and needs to be investigated further, as it can be due to a kidney or gallbladder problem. If you continually experience foamy urine, go and see your doctor.
Cloudy Urine: Milky urine can signal the presence of microscopic blood. It can also be caused by a urinary tract infection, bladder infection or kidney stones. Some sexually transmitted diseases such as gonorrhoea can change your urine colour. Vaginal discharge can also make the urine cloudy.
Black: Black colour may be due to chemicals and health issues. You must see your doctor and get it checked.
Jan 2017
Is it heartburn or heart attack?
Heartburn, also known as acid indigestion, is a burning sensation in the central chest or upper central abdomen. The pain often rises in the chest and may radiate to the neck, throat, or angle of the jaw. Heartburn is usually due to regurgitation of gastric acid (gastric reflux) into the oesophagus and is the major symptom of gastroesophageal reflux disease (GERD). In about 0.6% of cases it is a symptom of ischemic heart disease. Heartburn is discomfort or actual pain caused by digestive acid moving into the tube that carries swallowed food to your stomach (oesophagus).
The oesophagus is a tube that connects the mouth to the stomach. It is made of muscles that work to push food toward the stomach in rhythmic waves. Once in the stomach, food is prevented from refluxing (moving back into the oesophagus), by a special area of circular muscle located at the junction of the oesophagus and stomach, called the lower oesophageal sphincter (LES). A pressure difference across the diaphragm, the flat muscle that separates the chest from the abdomen, also tends to keep stomach contents in the stomach.
The stomach combines food, acids, and enzymes together to begin digestion. There are special protective cells that line the stomach to prevent the acid from causing inflammation. The oesophagus does not have this same protection, and if stomach acid and digestive juices reflux back into the oesophagus, they can cause inflammation and damage to its unprotected lining.
A burning sensation starting in the upper abdomen and moving up into the chest; Usually occurs after eating or while lying down or bending over; May awaken you from sleep, especially if you have eaten within two hours of going to bed; Usually relieved by antacids; May be accompanied by a sour taste in your mouth — especially when you're lying down; May be accompanied by a small amount of stomach contents rising up into the back of your throat (regurgitation).
Heartburn Causes
Risk factors include those that increase the production of acid in the stomach, as well as structural problems that allow acid reflux into the oesophagus. Some common foods that we eat and drink stimulate increased stomach acid secretion setting the stage for heartburn. Over-the-counter medications also may precipitate heartburn. Examples of these irritants include: alcohol, caffeine, aspirin, buprofen, carbonated beverages, acidic juices (grapefruit, orange, pineapple), acidic foods (tomatoes, grapefruit, and oranges), and chocolate.
Smoking and the consumption of high-fat content foods tend to affect function of the lower oesophageal sphincter (LES), causing it to relax from the stomach and allow acid to reflux into the oesophagus.
A hiatal hernia, where a portion of the stomach lies within the chest instead of the in abdomen, can affect the way the LES works and is a risk factor for reflux. Hiatal hernias by themselves cause no symptoms. It is only when the LES fails that heartburn occurs.
Pregnancy can cause increased pressure within the abdominal cavity and affect LES function and predispose it to reflux.
Obesity may also cause increased pressure in the abdomen, and thus reflux in the same way. Primary diseases of the oesophagus can also present with heartburn as a symptom. These include, among others, scleroderma and sarcoidosis.
Heartburn Symptoms:
Gastroesophageal reflux disease (GERD) is a condition in which heartburn is a symptom. Stomach acid refluxes up into oesophagus and causes pain. This pain can be felt as a burning sensation behind the sternum or breastbone, either as a spasm or a sharp pain. Many times the pain of acid reflux can be mistaken for the pain of a heart attack.
The pain of acid reflux (heartburn) can remain in the lower chest or it can radiate to the back of the throat and be associated with waterbrash, a sour taste in the back of the throat. If there is acid reflux near the larynx (voice box) in the throat, it may cause coughing episodes or hoarseness. Reflux over prolonged periods of time can be severe enough that acid wears away the enamel on teeth and causes decay.
Symptoms are often worsened after heavy meals, leaning forward, or lying flat. Those affected may often awaken from sleep with heartburn.
Complications
Heartburn is not without complications. If ignored, recurrent irritation and inflammation of the oesophagus can lead to ulcers, which are small areas of tissue breakdown. These can cause serious bleeding.
As well, scarring and stricture are other significant complications of GERD. Changes in the type of cells lining the oesophagus may result from acid reflux, causing a condition known as Barrett's oesophagus, which is associated with an increased risk of oesophageal cancer.
Heartburn Diagnosis
Heartburn is a common complaint, though it can be confused with other chest-related illnesses, including: heart attack, pulmonary embolus, pneumonia, and chest wall pain. The diagnosis begins with a complete history and physical examination. In many cases that provides enough information for the health care professional to make the diagnosis and begin a treatment plan. In some instances, further testing may be required:
X-ray: The patient may be asked to swallow barium or Gastrografin (two types of contrast materials) while a radiologist, using an X-ray or fluoroscopy machine, watches the contrast material travel down the oesophagus and enter into the stomach. Aside from looking for irregularities or inflammation within the oesophagus and of the oesophageal walls, this test can determine if the oesophagus muscles are working properly in a rhythmic fashion to push the contrast material into the stomach.
Endoscopy: In this test a gastroenterologist uses a flexible scope and with a fiberoptic camera to look at the lining of the oesophagus and stomach. Inflammation and ulcers can be identified. Biopsies and small bits of tissue can be obtained to look for cancerous or pre-cancerous cells.
Manometry and pH testing: Less commonly, when conventional therapy has failed to confirm the diagnosis, or when symptoms are atypical, use of pressure monitors and acid measurements from within the oesophagus may be helpful in making the diagnosis.
Heartburn Treatment
Lifestyle changes
Eat smaller, more frequent meals
Avoid eating before bedtime
Avoid alcohol, aspirin, ibuprofen, and caffeine
Stop smoking
Elevate the head of the bed (or use two or three pillows) to allow gravity to keep acid in the stomach and avoid acid reflux.
Heartburn Medication
Antacids may be taken after meals, at bedtime, or when needed, to bind excess acid in the stomach and to coat the oesophagus. Histamine H2 antagonists are medications that block the action of histamine (a chemical that stimulates stomach cells to produce acid) on the acid-producing cells of the stomach. This decreases acid production to hopefully decrease symptoms. Examples include: cimetidine (Tagamet), ranitidine (Zantac), and famotidine (Pepcid). Some H2 blockers and proton pump inhibitors are available OTC without a prescription. However, there may be potential interactions with some prescription medications. Check with your health care professional or pharmacist for advice about their safe use. Proton pump inhibitors (PPIs) are another class of drugs that block the production of acid by the stomach. PPIs include: Omeprazole (Prilosec, Rapinex), rabeprazole (Aciphex), pantoprazole (Protonix), lansoprazole (Prevacid), and esomeprazole (Nexium).
Heartburn Surgery
Surgery is an option for those patients for whom intensive medical therapy does not provide adequate relief, with Barrett's oesophagus, with reflux so severe that it causes hoarseness, pneumonia, or wheezing. Different surgical approaches to oesophageal reflux are available. In fundoplication, the stomach is wrapped around the lower oesophagus, in effect creating a new physiologic valve to take the place of the lower oesophageal sphincter. New devices have been recently approved that can be wrapped around the lower oesophagus that act link the LES. The specific procedure will be recommended based upon the patient's situation.
What signs and symptoms are more likely to occur with a heart attack than with heartburn?
The "textbook" heart attack involves sudden, crushing chest pain and difficulty breathing, often brought on by exertion. Many heart attacks don't happen that way, though. The signs and symptoms of a heart attack vary greatly from person to person. Heartburn itself can accompany other symptoms of heart attack. Typical heart attack signs and symptoms include: Pressure, tightness, pain, or a squeezing or aching sensation in your chest or arms that may spread to your neck, jaw or back. Nausea, indigestion, heartburn or abdominal pain. Shortness of breath. Cold sweat. Fatigue. Light-headedness or sudden dizziness. If there is no shortness of breath and sweating, it is more likely to be heartburn, but medical advice should be sought.
Dec 2016
Facts about bleeding in the digestive tract
Gastrointestinal (GI) bleeding is any type of bleeding that starts in one’s GI tract, also known as the digestive tract. Such bleeding is a symptom of a disease or a condition, rather than a disease or a condition itself. Acute GI bleeding is sudden and can sometimes be severe. Chronic GI bleeding is slight bleeding that can last a long time or may come and go. GI bleeding is also called bleeding in the digestive tract, upper GI bleeding, or lower GI bleeding. The upper GI tract and lower GI tract are different areas of your GI tract.
Symptoms of GI Bleeding
Symptoms of gastrointestinal (GI) bleeding may include black or tarry stool, bright red blood in vomit, cramps in the abdomen, dark or bright red blood mixed with stool, dizziness or faintness, feeling tired, paleness, shortness of breath, vomit that looks like coffee grounds and weakness. While the above-mentioned are the common symptoms of GI bleeding, acute bleeding can even make one go into shock. It is thus an emergency condition and its symptoms include a drop in blood pressure, little or no urination, rapid pulse and unconsciousness. Then there is chronic bleeding and one can develop anaemia as a result of this condition. Symptoms may include feeling of tiredness and shortness of breath and these symptoms can develop over time. Some people may have occult bleeding. Occult bleeding may be a symptom of inflammation or a disease such as colorectal cancer. A simple lab test can detect occult blood in your stool.
Causes of GI bleeding
There are a number of conditions that can cause GI bleeding. A medical expert can try to find the cause of such bleeding by finding its source. The following conditions may include possible causes of GI bleeding:
Angiodysplasia: Angiodysplasia is when you have abnormal or enlarged blood vessels in your GI tract. These blood vessels can become fragile and bleed.
Benign tumors and cancer: Benign tumors and cancer in the oesophagus, stomach, colon, or rectum may cause bleeding when they weaken the lining of the GI tract. A benign tumour is an abnormal tissue growth that is not cancerous.
Colitis: Ulcers in the large intestine are a complication of colitis. Ulcerative colitis is an inflammatory bowel disease that can cause GI bleeding.
Colon polyps: Colon polyps can cause GI bleeding. One may have more than one colon polyp at a time. Some types of polyps may be cancerous or can become cancerous.
Diverticular disease: Diverticular disease can cause GI bleeding when small pouches, or sacs, form and push outward through weak spots in your colon wall.
Oesophageal varices: Oesophageal varices can cause GI bleeding. Oesophageal varices are usually related to a chronic liver condition called cirrhosis.
Esophagitis: The most common cause of esophagitis is gastroesophageal reflux (GER). GER happens when your lower oesophageal sphincter is weak or relaxes when it should not. Stomach acid can damage your oesophagus and cause sores and bleeding.
Gastritis: Some common causes of gastritis include the use of nonsteroidal anti-inflammatory drugs (NSAIDs) and other medicines; infections; Cohn’s disease; serious illnesses and severe injuries. If untreated, gastritis can lead to ulcers or worn-away areas of the stomach lining that can bleed in your GI tract.
Haemorrhoids or anal fissures: Haemorrhoids can cause GI bleeding. Constipation and straining during bowel movements cause haemorrhoids to swell. Haemorrhoids cause itching, pain, and sometimes bleeding in your anus or lower rectum. Anal fissures are small tears that also can cause itching, tearing, or bleeding in your anus.
Mallory-Weiss tears: Severe vomiting may cause Mallory-Weiss tears, which can cause GI bleeding. You can have more than one Mallory-Weiss tear at a time.
Peptic Ulcers: The bacteria Helicobacter pylori (H. pylori) and use of nonsteroidal anti-inflammatory drugs (NSAIDs) can cause peptic ulcers. Peptic ulcers can wear away your mucosa and cause GI bleeding.
Diagnosis of GI Bleeding
To diagnose gastrointestinal (GI) bleeding, a doctor will first find the site of the bleeding based on a patient’s medical history—including what medicines he is taking—and family history, a physical exam, and diagnostic tests. During a physical exam, a doctor most often examines one’s body, listens to sounds in the abdomen using a stethoscope and taps on specific areas of the body. Depending on the symptoms, the doctor will order one or more diagnostic tests to confirm whether a person has GI bleeding and, if so, to help find the source of the bleeding.
Tests to diagnose GI bleeding
The doctor may perform certain tests and procedures to diagnose the cause of GI bleeding. These may include:
Stool tests: A stool test is the analysis of a sample of stool. The doctor will give one a container in which to catch and store the stool. Stool tests can show occult bleeding.
Blood tests: The medical expert may take a blood sample from you and send the same to a lab for test. The blood test can help determine the extent of your bleeding and whether you have anaemia.
Gastric lavage: A gastric lavage is a procedure in which a doctor passes a tube through your nose or mouth into your stomach to remove your stomach contents to determine the possible location of your GI bleeding. A doctor may also use gastric lavage to help prepare for another diagnostic test or, most often, for acute, severe bleeding. The doctor performs this procedure in an outpatient centre or a hospital. You most often receive a liquid anaesthetic to numb your throat.
Endoscopy: Endoscopy procedures involve a doctor examining a hollow passage in your body using a special instrument. An endoscopy procedure may help your doctor see if and where you have GI bleeding and the bleeding’s cause. Doctors most often use upper GI endoscopy and colonoscopy to test for acute GI bleeding in the upper and lower GI tracts.
Upper GI endoscopy: In an upper GI endoscopy, your doctor feeds an endoscope down your oesophagus and into your stomach and duodenum. A trained specialist performs the procedure at a hospital or an outpatient centre. You most often receive a liquid anaesthetic to numb your throat and a light sedative to help you stay relaxed and comfortable during the procedure.
Enteroscopy: During an enteroscopy, a doctor examines your small intestine with a special, longer endoscope.
Capsule endoscopy: In capsule endoscopy, you swallow a capsule containing a tiny camera that allows your doctor to see inside your GI tract. You don’t need anaesthesia for this procedure. As the capsule passes through your GI tract, the camera will record images that your doctor later downloads and reviews. The camera capsule leaves your body during a bowel movement.
Colonoscopy: Colonoscopy is a procedure in which a doctor uses a long, flexible, narrow tube with a light and tiny camera on one end, called a colonoscope or scope, to look inside your rectum and colon. A trained specialist performs a colonoscopy in a hospital or an outpatient centre. You will receive sedatives, anaesthesia, or pain medicine during the procedure. The doctor can see and treat any GI bleeding during a colonoscopy.
Flexible sigmoidoscopy: Flexible sigmoidoscopy is a procedure in which a doctor uses a flexible, narrow tube with a light and tiny camera on one end, called a sigmoidoscope or scope, to look inside your rectum and sigmoid colon and treat any bleeding. A trained specialist performs a flexible sigmoidoscopy at a doctor’s office, a hospital, or an outpatient centre. You do not need anaesthesia for this procedure.
Treatment of GI bleeding
Treatment of gastrointestinal (GI) bleeding depends on the cause and location of your bleeding. During an upper GI endoscopy, a lower GI endoscopy, a colonoscopy, a flexible sigmoidoscopy, or a laparotomy, a doctor can stop the bleeding in your GI tract. He or she can stop the bleeding by inserting tools through an endoscope, colonoscope, or sigmoidoscope to inject medicines into the bleeding site and treat the bleeding site and surrounding tissue with a heat probe, an electric current, or a laser to close affected blood vessels with a band or clip. During an angiogram, a radiologist can inject medicines or other materials into blood vessels to stop some types of bleeding. When infections or ulcers cause bleeding in your GI tract, health care professionals prescribe medicines to treat the problem. When a person has severe or acute bleeding or bleeding that does not stop, a surgeon may need to perform a laparoscopy or a laparotomy to stop the bleeding.
Prevention of GI bleeding
Doctors can prevent GI bleeding by treating the conditions that cause the bleeding. You can prevent some of the causes of bleeding in your GI tract by limiting the amount of nonsteroidal anti-inflammatory drugs (NSAIDs) you take or by talking with your health care professional about other medicine options and following your doctor’s recommendations for treatment of gastroesophageal reflux (GER).
Keep warm, eat warm & exercise to keep indigestion at bay - November 2016
Changing season brings on a deluge of ailments, often flues and viral. But one part of our anatomy that suffers with each onslaught of illness is our stomach or the digestive system. The digestive system can be a source of considerable illness in the winter season if people eat wrong foods or don’t keep warm. Generally, the digestive system enters an active stage in winter and that's why dietary reinforcements are usually more effective than in other seasons. But stomach problems also often occur due to cold air, eating unsafe foods or spicy foods and drinking impure water. Though cold air arouses people's desire to eat more food, it also largely increases gastric acid, which may pose a threat to the gastric mucosa. There is a high recurrence of chronic stomach problems like ulcers in the winter season and some patients may even suffer from stomach bleeding. In addition, the cold environment may also arouse uncomfortable stomach contractions. One other factor responsible for the winter discomforts is a lack of activity as people keep indoors or snuggle in bed while wanting to eat all kinds of foods from groundnuts to grand three-course meals. This can cause improper digestion of the food consumed thus leading to stomach aches.
Indigestion is a condition when there is discomfort or pain in the chest, or upper abdomen though it cannot be considered as a disease. But the digestion process is really important as it churns the actual food to convert it into energy. This in turn helps an individual maintain perfect body metabolism. Indigestion may take place immediately after eating meals. It happens when the acids from the stomach returns to the mouth which takes place when the valve of the stomach does not function properly. GERD or gastro-esophagealreflux disease is the medical term for this condition. Here the food is not digested in a proper way which gives rise to acidic feeling, bloating or discomfort.
Symptoms of indigestion include nausea and vomiting, feeling full often termed as bloating, belching and gas, burning sensations in the upper abdomen, acidic taste after eating, abdominal pain and discomfort or growling stomach. Medical attention is essential when long term indigestion is accompanied with weight loss, severe pain that gets worse, or when there is blood in vomit.
Heartburn or a burning sensation in the chest is the most common symptoms of acidity during winter. At times this burning sensation may be accompanied with mild or moderate stomach pain. Sometimes the stomach pain may become unbearable, indicating severe acidity. In the milder form, people may also experience dryness of throat. Likewise, people may even continuously eject gas from the mouth or anus. People prone to acidity may tend to get more acidity in winter especially after a heavy meal. Acidity during winter in many cases does not have any serious medical consequences. In most cases, acidity is triggered when people sleep just after having dinner. Many people also get acidity for eating excessive fried or spicy food. Eating excessive chocolates or foods containing huge amount of fats can also lead to acidity in winter. To beat the chill outside, many people consume excess amount of caffeine drinks and alcoholic beverages, which in turn leads to symptoms of acidity. Citrus fruits are available in plenty during the winter season and consuming these fruits in excess amount can also lead to acidity during winter months. Whether it is winter or any other season of the month, it is important to keep a check on weight, as obese people are more prone to this condition. Hiatus hernia is a condition when the part of the stomach moves towards the chest causing heart burn. Acute pancreatitis when there is inflammation of the pancreas and acute gastritis when there is inflammation of the stomach also leads to indigestion. Food poisoning and infection in the stomach create symptoms of indigestion. People suffering from diabetes often face the problem of gastro paresis which is a condition where the stomach is not cleared properly. Most pregnant women suffer from indigestion which are said to be caused by high levels of female hormones during pregnancy.
Indigestion can be controlled by reducing the intake of fatty foods, coffee, tea and alcohol, giving up smoking, sleeping with the head rose to reduce pressure on the stomach, reducing stress levels by adopting relaxation methods like meditation, yoga and deep breathing, food must be eaten slowly and evening meals should be taken 2-3 hours before sleeping. There are some medicines like antacids which can be taken to reduce the symptoms of indigestion.
Wearing enough clothes and avoiding cold environments shortly after eating are good strategies for protecting the stomach, especially for people with chronic problems, but some form of exercise or movement is also necessary. As the stomach is close to the abdominal wall, with little protection from surrounding muscle or fat, pathogenic cold may easily result without proper insulation. Also, cold food should be avoided in winters to reduce stimulation of gastric fluids, especially at breakfast. As most of the organs are still in a state of sleep, eating cold foods may result in contraction and poor blood circulation in the digestive system, leading to indigestion. Warm or relatively hot foods, however, can help stimulate blood circulation and wake up the organs. Wearing a belly belt can also help protect the stomach from the cold. Warming fruit with hot water, or briefly boiling it, before eating can also be done. Generally, the antioxidant like polyphenol in fruit won't be damaged at 100 degrees Celsius. Boiled fruits will effectively nourish organs, move bowels and promote digestion, as well as reduce possible stimulation in the stomach. But foods rich in vitamin C, such as kiwi, orange, pomelo and strawberry, should not be boiled for long, as the temperature may destroy the vitamin. We must not heat these fruits for more than five minutes. Adding a little spice in food can help warm up and improve the appetite, but too spicy foods will only arouse too much stimulation to the stomach and cause problems. For those who rarely eat spicy foods, digesting a large amount at once may lead to acute stomach inflammation.
And since immunity decreases with cold temperatures, we should also be aware of infectious digestive ailments with typical symptoms like diarrhoea and vomiting. Uncooked foods are the first group recommended to be crossed off the menu. Hot pots, many people's favourite in the season, are also not advisable because dipping the food in boiling water may not be enough to kill off any germs. Most people prefer tender meats without long heating but the cost may be high as they are much more dangerous than well-cooked ones. Warm foods are more recommended in the season. It is also advised to add spleen-benefiting herbs like barley to food, especially soups.
Cabbage is an excellent source of vitamin C. It also contains significant amounts of glutamine, an amino acid which has anti-inflammatory properties. Cabbage can also be included in dieting programs, as it is a low-calorie food. In European folk medicine, cabbage leaves are used to treat acute inflammation. Fresh cabbage juice has been shown to promote rapid healing of peptic ulcers. As for patients with chronic stomach problems like inflammation or ulcers, it is essential to quit smoking, drinking and eating other stimulating foods as well as avoid bad moods and fatigue. It is also advised to take precautionary medicine to stop relapses of stomach problems. See a doctor if you have stomach pains as taking medicine without professional advice may aggravate the problem. For example, people may take painkillers for stomach pain but some could cause adverse reactions or even ulcers and bleeding.
If indigestion is mild and infrequent, it does not require any health consultation. However, if you are suffering from it more often, a health check is mandatory. Depending upon the type of indigestion which is governed by the symptoms, further investigation is also done. Endoscopy is done to examine the inside of your body using a thin, flexible tube having camera to visualize from the images. Simply pain in the stomach is not treated as indigestion. Your doctor will go through detailed set of steps and advise X-rays of stomach (even barium meal X-ray) or small intestine, or even an ultrasound scan. Usually normal conditions of indigestion do not require any tests, but if the conditions persist, tests are prescribed to detect the bacteria that causes peptic ulcer.
Malaria, dengue or chikungunya- know the difference - October 2016
Malaria, dengue, and chikungunya are three types of mosquito-borne diseases. Because the symptoms are so similar, it becomes difficult at times to make a conclusive identification without laboratory testing. Although these diseases have almost identical manifestations, it is crucial to differentiate them for proper treatment. For example, both dengue and chikungunya are viral diseases whose vector is the Aedes aegypti mosquito. Chikungunya has as an additional vector, the Asian tiger mosquito (Aedes albopictus). Chikungunya is a problem in Southeast Asia, as is dengue, but also in India and sub-Saharan Africa. Dengue and chikungunya have much in common in terms of symptoms, incubation period, clinical course, vector, and geographical distribution. A key feature shared by both diseases is that the fever comes on sharply about a week after exposure and lasts about a week before resolving. Joint pain is the difference between the two. In adults, the arthritis can go on for many months.
KNOW WHAT CAUSES MALARIA
Malaria is caused by plasmodium, a single-celled parasite often transmitted by infected mosquitoes. The parasite is injected into a person’s circulatory system through the saliva of the mosquito. It then travels to the liver where it will mature and reproduce. When the plasmodium matures, it will infect red blood cells until they burst. Then, newly developed plasmodium from the red blood cells will spread, and infect more red blood cells. Symptoms: In most cases, the manifestations of malaria will begin 8-25 days after the mosquito bite. The severity of the signs and symptoms of malaria may depend upon three factors: the type of malaria, your immune system, and health of your spleen. There are 5 types of malaria. These include P. Vivax, P. Malaria, P. Ovale, P. Falcifarum, and P. Knowlesi. During a malaria infection, red blood cells rapidly die, and the spleen may not be able to keep up with the demand, leading to sepsis and organ failure. High fever is very common in malaria patients. The temperature may reach as high as 40 °C (104 °F). The fever is often accompanied by chills and then sweating. The doctor will get a blood test done to confirm malaria.
KNOW WHAT CAUSES DENGUE
There are four types of dengue viruses, all of which are spread by mosquito. When a mosquito is infected by the virus, it will spread the virus through its saliva when it bites. Dengue can also be transmitted from human to human. For example, infected blood used in a blood transfusion can cause dengue. Even organ donation and mother to child transmission are possible. Symptoms: The incubation period of dengue (period before which symptoms are visible) is about 3-14 days. Your symptoms may vary, depending upon the type of the virus and your level of immunity. The virus will circulate around your body after infection, attacking white blood cells and other antibodies, which will compromise your immune system. The virus will further replicate within the cell until the cell bursts and dies, releasing cytokines that initiate the inflammatory response of the body as it tries to ward off the virus. The death of the white blood cells will trigger leakage of other fluids from the cells, leading to hypoproteinemia (low protein), hypoalbuminema (low albumin), pleural effusion (fluid in the lungs), ascites (fluid in the stomach area), hypotension (low blood pressure), shock, and even death. A high fever will take place as a result of the body’s effort to suppress the virus. Take note of an intense headache and backache. There is pain behind your eyes. The pain is characterized as dull and deep. Widespread bleeding can occur, because the virus attacks your capillaries, the smallest blood vessels in the body. During a severe case, bleeding is more common in the nose and gums. Your pulse may also become weak. As your fever decreases, skin rashes may start to appear. The rash is reddish, an















Leave a comment